Many people
have had the flu at last once in their life and see their doctors every year
for a flu vaccination. The vaccine is
typically trivalent, which means that it protects against three different
strains of the influenza virus: H1N1, H3N2, and an influenza B strain. This vaccine is given as an intradermal shot
meaning it is injected into the skin instead of the muscle2. Seeing as how flu season is fast approaching
I though it fitting to bring to light an article relating the flu, or more
specifically the pandemic influenza A virus strain (pH1N1) of the 2009-2010 flu
season. However, before delving into the
article I would like to provide the basic, necessary background information.
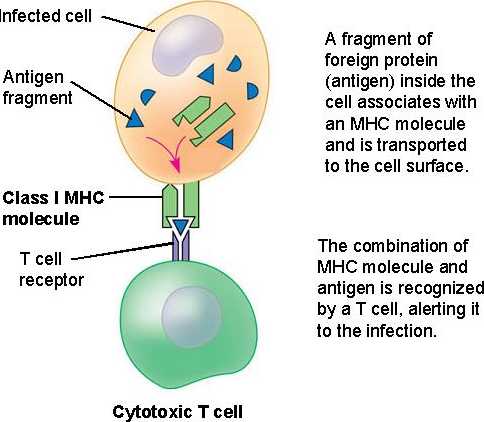
When an
antigen is engulfed by an antigen presenting cell (APC), its proteins are
broken down and a small peptide chain of about 10 base pairs is expressed so
that activated cytotoxic T-cells can destroy the infected cell3. The proteins that express these peptides are
called MHC (major histocompatabiltiy complex) class I and MHC class II proteins
which are encoded by the human leukocyte antigen (HLA) gene3. For MHC class I gene on HLA there are three
regions: HLA-A, HLA-B, and HLA-C for which many different alleles exist3. Some MHC alleles display the peptides for
T-cell recognition better than others which is why different people have
different immune responses to the same pathogen.
Additionally, CD8+ is the specific receptor that MHC class I
binds to on T-cells3.
Infected cells also release interferons (INFs) that increases the
expression of MHC molecules which helps to fight off infection by causing more
interactions with T-cells3.
The first section
of this article demonstrated that the ability of HLA to create MHC molecules to
express pH1N1 is related to the CD8+ T-cell response. The efficiency score, the ability for a
peptide of pH1N1 to be expressed on the cell surface, for 95 common alleles of
HLA-A and HLA-B was computed for pH1N11. Samples from 13 individuals were taken and
the participants were ranked according to their average efficiency score for
pH1N1. The samples were then infected
with different strains of influenza and the frequency of INF-
γ production was correlated with efficiency score1. Interestingly, age and gender didn’t appear
to have any correlation.
The
second section of the article looked at different alleles and their mortality
rates for pH1N1. 95 of the most common
HLA class I alleles were studied against many different strains of
influenza. A majority of the alleles
demonstrated a preference to bind to pH1N1; however, A*24 alleles didn’t bind
well to pH1N1 as seen with their negative efficiency scores1. This could mean that people with A*24 alleles
are more likely to develop severe cases of pH1N1. Additionally, there was a positive
correlation with mortality rate. Further
analysis of the different alleles showed that A*68 and B*39 alleles were also
positively correlated with mortality rate while A*32 alleles were negatively
associated with mortality rate1.
The
third and final portion of the essay discussed the high rate of HLA-A*24
alleles within native populations. Even
though native people account for only a small percentage of the population,
fewer than 5%, they represented almost 18% of all hospitalization cases in
Arizona1. This further
supports the claim of this paper: that there is a correlation between HLA
allele targeting efficiency and mortality rates.
This study
indicates that when it comes to H1N1, there are certain alleles for MHC that
can be extremely helpful or have little effect when fighting of the flu. Also, the alleles you have could put you at
greater risk for developing a severe case of H1N1. Hopefully you will avoid the flu this season,
and to help you do so keep these tips in mind:
Primary Source:
1. Hertz, Tomer, et al. "HLA Targeting Efficiency Correlates with Human T-cell
Response Magnitude and with Mortality from Influenza A Infection." Proceeding
of the National Academy of Sciences 110.33 (2013): 13492-3497. Web.
Secondary Sources:
2. "Key Facts About Seasonal Flu
Vaccine." Centers for Disease Control and Prevention. Centers for
Disease Control and Prevention, 25 Sept. 2013. Web. 30 Sept. 2013. < http://www.cdc.gov/flu/protect/keyfacts.htm>
3. Mak, Tak W., and Mary E. Saunders. Primer
to the Immune Response: Academic Cell Update. Burlington: Elsevier, 2011.
Print.
Images:
http://bio1152.nicerweb.com/Locked/media/ch43/t_cells.html
http://www.fda.gov/forconsumers/consumerupdates/ucm092805.htm

No comments:
Post a Comment